Walmart is helping fight the opioid crisis. We are proud of our pharmacists, who help patients understand the risks about opioid prescriptions. And our pharmacists have refused to fill hundreds of thousands of opioid prescriptions they thought could be problematic.
On top of that, Walmart has blocked thousands of questionable doctors from having their opioid prescriptions filled by any of our pharmacists, as part of our good-faith efforts to help address the opioid crisis.
As a result, many health regulators, medical groups, doctors and patients say that Walmart is going too far in refusing to fill opioid prescriptions—and even say we are improperly interfering in the doctor-patient relationship and potentially harming patients who need their medicine.
This is a big reason why plaintiff-lawyer driven lawsuits brought around the country against Walmart and other pharmacies are misguided and dangerous to public health. In search of deep pockets, plaintiffs’ lawyers representing cities, counties and others are pushing a legal theory that pharmacies should be held responsible for the opioid crisis. In fact, courts around the country have rejected plaintiffs’ novel “public nuisance” liability theories in lawsuits in Arkansas, Connecticut, Delaware, Illinois, California, Oklahoma, North Dakota and South Dakota. As the Wall Street Journal said, it makes no sense to punish pharmacies for “filling legal prescriptions for a legal substance for real patients from licensed doctors.”
One serious and big-picture problem with the plaintiffs’ attempt to turn pharmacists and pharmacies into the “doctor police” is that it forces them to come between doctors and their patients in a way Congress never intended, and federal and state health regulators say isn’t allowed. And many patients say that pharmacies are preventing them from getting needed medicine.
The Lawsuits: Putting Pharmacists Between a Rock and a Hard Place
Think about what happens when a patient brings an opioid prescription from a doctor into a pharmacy to fill.
Pharmacists aren’t doctors and don’t write opioid prescriptions. Instead, when a patient hands an opioid prescription written by a state licensed and DEA-approved doctor to a pharmacist, a pharmacist has to decide whether to fill it. No one disputes that if a pharmacist knows a prescription is fake or forged, she shouldn’t fill it.
The plaintiffs’ lawsuits raise a different issue: What should a pharmacist do with a prescription that is valid on its face and written by a state-licensed and DEA-approved doctor?
For a prescription like that, should a pharmacist accept the doctor’s medical judgment and fill the prescription? Or should a pharmacist second-guess the doctor and not fill it, leaving the patient without the medicine prescribed by her doctor? Remember, a pharmacist must make this decision without the benefit of a medical degree, without examining the patient, and without access to the patient’s medical records.
Either decision carries risks with it “the sword of Damocles hanging over Walmart and its pharmacists.”
If a Pharmacist ...
Fills a Prescription
If a pharmacist accepts a doctor’s judgment and fills a valid-looking prescription written by a state licensed and DEA-approved doctor, then under the plaintiffs’ theory, she and the pharmacy still face civil liability based on plaintiffs’ experts’ hindsight assessment that the prescription should not have been filled.
One reason these lawsuits are so wrong-headed is because no law tells a pharmacist how to decide whether to fill a prescription. Instead, in these lawsuits, plaintiff lawyers second-guess pharmacists for not second-guessing doctors. That moves health care decisions into a courtroom and further and further away from patients and doctors.
Refuses to Fill a Prescription
On the other hand, if a pharmacist refuses to fill the same prescription, state boards could investigate her for the unauthorized practice of medicine and even take away her license. And patients and doctors could sue her for not filling opioid prescriptions. And she could harm patients who need the medicine.
These aren’t hypothetical risks—they are happening all over the country. And pharmacies are also sued, investigated and criticized for instructing pharmacists not to fill any opioid prescriptions from certain doctors.
Patients
In fact, a class action lawsuit says pharmacies are harming patients and illegally discriminating against them by not filling needed opioid prescriptions.
Even the DEA has expressed concern that “legitimate patients” are sometimes unable to “get their prescription for pain medications filled at large retail pharmacies.”
State Medical and Pharmacy Boards
In addition to patient criticisms, state medical and pharmacy boards all over the country have criticized, investigated and threatened Walmart and our pharmacists for going too far in refusing to fill opioid prescriptions.

Complaints against Walmart and its pharmacists for refusing to fill opioid prescriptions have also been filed with, or pursued by, many Boards of Pharmacy or Medicine across the country, including those in dark blue above.
Below are just a few examples:
- A Georgia legislator proposed a bill to punish Walmart for blocking questionable doctors from having their opioid prescriptions filled, saying Walmart is “interfering with the doctor patient relationship.”
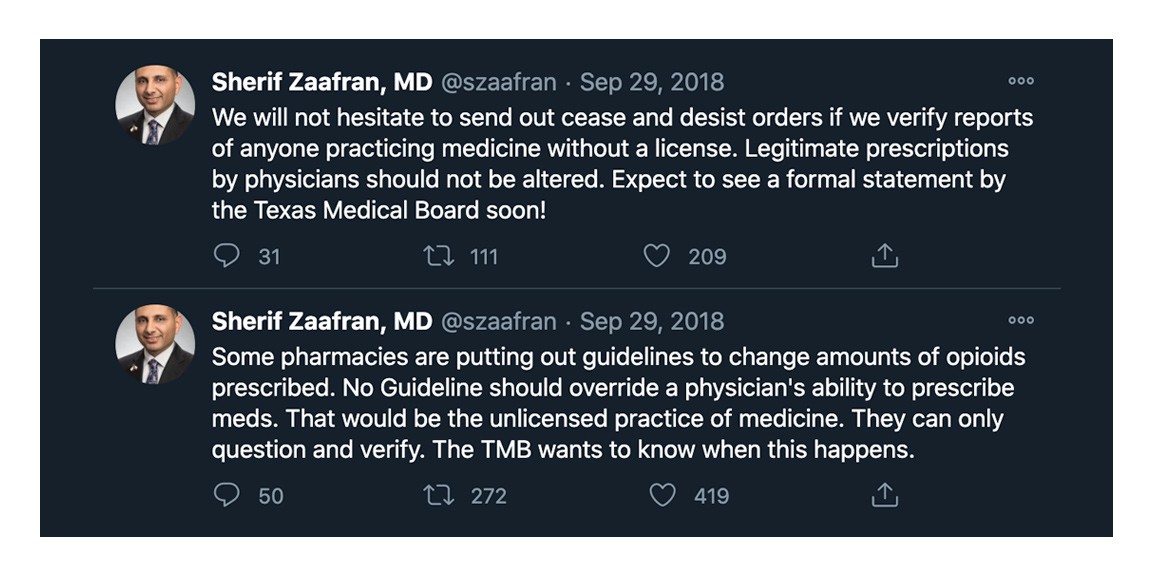
- The President of the Texas Medical Board threatened cease-and-desist orders against Walmart and our pharmacists for interfering in the practice of medicine by not filling certain opioid prescriptions.
- Citing Tennessee law, the Tennessee Pharmacy Board launched inspections of Walmart pharmacies and opened a months-long investigation after a doctor complained Walmart wouldn’t allow its pharmacists to fill the doctor’s opioid prescriptions.
The list goes on, and you can read more examples in this news story or in this legal filing by Walmart.
Federal Health Agencies
Pharmacists and pharmacies also get contradictory guidance from federal health agencies and even the DEA that often disagrees with the plaintiffs’ theory that pharmacists should interfere with a doctor’s individualized medical judgment. Here are just a few examples, but there are many more.
- Medical associations cite the Health and Human Services Department’s statement that doctors and patients—not pharmacists—should be the ones making the decisions.
- At the same time the Department’s lawsuit says Walmart should have been blocking more doctors and prescriptions. Recently, the DEA said that the agency has no legal authority to regulate “the general practice of medicine” and that federal law doesn’t include specific number limits on prescriptions.

Doctors
And it’s not just state and federal health regulators saying pharmacists and pharmacies are going too far in refusing to fill opioid prescriptions—doctors are also weighing in.
For example, the American Medical Association said Walmart “disrupted legitimate medical practices” by refusing to fill opioid prescriptions from certain doctors.

The AMA has also accused the company of creating a physician “blacklist.”

Many doctors have sued pharmacists and pharmacies—including Walmart—for blocking their prescriptions, saying they have tarnished their professional reputations. And recently, a doctor in Nevada sued Walmart and other pharmacies saying they acted improperly in “issu[ing] blanket edicts refusing to fill narcotic prescriptions from certain medical providers.” In a similar lawsuit, a federal judge recently ordered one pharmacy to fill prescriptions for a doctor that the pharmacy had blocked.
There are many other examples, but you get the picture: plaintiffs’ legal theories are trying to put pharmacists and pharmacies between a rock and a hard place by demanding they go further in second-guessing doctors, while state health regulators say they are going too far. Ultimately, patients are caught in the middle.
A Better Path: Clarity for Doctors, Patients and Pharmacists
Walmart is proud of our pharmacists, and we intend to defend against these meritless lawsuits. We also need a real solution to the rock-and-a-hard-place problem. In working toward the best policy answer for this problem, each branch of government has a role to play in providing clarity for doctors, patients and pharmacists on how to handle opioid prescriptions.
What DOJ and DEA Can Do
For starters, DOJ and DEA could go through the proper rulemaking channels to clarify going forward what the agencies expect of pharmacies and pharmacists, rather than make them guess what DEA wants by looking at DEA’s scattered letters and PowerPoints (that have no legal authority, anyway). In fact, Walmart has filed a petition asking DEA to propose a rule-making to provide this much needed clarity.
And according to the Department’s own Inspector General, DEA needs to do a better job using the tools and legal authority Congress gave it to keep bad doctors from prescribing opioids. Right now, the plaintiffs’ lawsuits are trying to turn pharmacists and pharmacies into the prescriber police—even though they lack DEA’s authority and tools to do their job, and states say that they can’t under state law.
What Legislatures Can Do
Legislatures—state and federal—also have an important role. That’s why Walmart has been pressing for much-needed legislative reforms to help fix the opioid crisis. For example, legislatures could help protect pharmacists when they properly refuse to fill prescriptions, so they do not face retaliatory investigations and lawsuits—protections we have asked for in Georgia, for example.
What Courts Can Do
And the courts need to clarify what existing law says. That is why in 2020, Walmart proactively brought its own lawsuit, asking a court for clarification on what the law says pharmacists and pharmacies should do when a patient presents an opioid prescription that looks legitimate. Walmart also sent the DEA a formal legal request that it live up to its legal responsibility and provide guidance to the pharmacy industry.
Our nation’s doctors, pharmacists and patients deserve better than the current bramble patch of inconsistent, conflicting and outright contradictory guidelines from federal and state regulators. And, we shouldn’t trust that plaintiffs’ lawyers, with their own motivations, will lead us to a solution that is good for health care. Let’s work together to fix this.



